Itaconate is a negative regulator of inflammation
Glucose metabolite reduces inflammation
A new study suggests that a glucose metabolite called itaconate functions as a negative regulator of macrophages (a type of immune cells). Macrophages can cause inflammation. This study reveals that itaconate is critical for the activation of the anti-inflammatory pathways in macrophages[1].
The study is conducted by an international team consisting of researchers from Trinity College Dublin in Ireland, University of Oxford, University of Dundee, University of Cambridge, University of Glasgow in the UK, Harvard Medical School in the USA, and GlaxoSmithKline R&D in Germany.
Itaconate is a molecule derived from glucose, the most important source of energy in the body. Although itaconate is one of the most highly induced metabolites in activated macrophages, its functions have not been well studied. Recent studies suggest itaconate as a regulator of macrophage function.
The current study uncovered that itaconate acts as a brake on macrophages, reducing inflammation. Working with human cells and mouse models, the team found that itaconate is involved in the activation of the anti-inflammatory transcription factor Nrf2 by lipopolysaccharide in mouse and human macrophages. Macrophages convert glucose into itaconate, which leads to reduced production of inflammatory factors. Mechanically, itaconate directly modifies proteins via alkylation of cysteine residues. This action enables the transcription factor Nrf2 to increase the expression of genes associated with anti-oxidant and anti-inflammatory effects. These results imply that itaconate is an important anti-inflammatory molecule and it acts via Nrf2 to limit inflammation.
Findings of this study have been published in a paper titled 'Itaconate is an anti-inflammatory metabolite that activates Nrf2 via alkylation of KEAP1,' appearing in Nature this week.
Itaconate and anti-inflammatory mechanisms identified in this study could be targeted to develop novel anti-inflammatory drugs. Dr. Luke O'Neill, corresponding author of the study, hopes this study would have implications for treatment of some currently hard-to-treat diseases.
Dr. O'Neill and his colleagues have been studying the molecular basis of innate immunity and inflammation for years. Their recent research interests include metabolic changes in macrophages.
Some other studies have shown that itaconate regulates macrophage metabolism and effector functions and that itaconate exerts anti-inflammatory effects when administered in vitro and in vivo during macrophage activation and ischemia-reperfusion injury. The evidence highlights itaconate as a major physiological regulator of the metabolism and function of inflammatory macrophages.
The current study further proves the anti-inflammatory function of itaconate and reveals a molecular mechanism of how itaconate exerts anti-inflammatory effects, which could help to design anti-inflammatory drugs. It appears that itaconate limits inflammation via the transcription factor Nrf2. Nrf2, also known as
NFE2L2, is a member of a small family of basic leucine zipper (bZIP) proteins and regulates the expression of antioxidant proteins that protect against oxidative damage triggered by injury and inflammation.
Functions of macrophages
Macrophages are a type of white blood cells. Their main function is to detect, engulf and destroy cellular debris, damaged or abnormal cells, and foreign substances like pathogens. These cells take part in antigen presentation, phagocytosis, and immunomodulation.
Compared with normal cells, macrophages are much bigger in size, with a diameter of about 21 micrometers. The term 'macrophage' is formed by the combination of the Greek terms 'makro', which means big, and 'phagein', which means eat. So, literally, macrophages refer to big eaters.
Macrophages are an essential part of the innate and acquired immune systems, protecting the body against pathogens and illnesses. In addition, macrophages also function as key regulators of embryogenesis, organogenesis, as well as tissue growth. Recent evidence supports a role of macrophages in tissue regeneration and self-renewal. Tumorigenesis may also involve macrophages, and therefore, targeting macrophages is a potential therapeutic strategy[2].
Stimulated macrophages can secrete a variety of molecules, such as cytokines, chemokines, leukotrienes, prostaglandins, and complement to modulate the immune response and other cellular activities.
Macrophages exist in nearly all tissues and are produced through differentiation of monocytes, one of the major groups of circulating white blood cells. When there is tissue damage or infection, the monocytes leave the blood and travel to the affected tissue and develop into macrophages. These macrophages can change their structures to perform different functions.
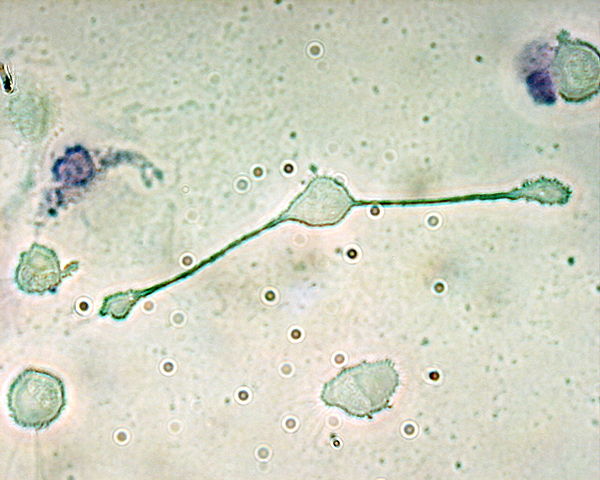
Fig. 1 A macrophage stretching its arms to engulf particles
(By The original uploader was Obli at English Wikipedia. - Transferred from en.wikipedia to Commons., CC BY-SA 2.0, https://commons.wikimedia.org/w/index.php?curid=635700)
Types of macrophages
Macrophages can be classified into two groups, M1 and M2, based upon their polarization. M1 macrophages encourage inflammation, whereas M2 macrophages decrease inflammation.
M1 macrophages are typically activated by
IFN-γ or lipopolysaccharide (LPS). These macrophages produce nitric oxide (NO) or reactive oxygen intermediates (ROI) to protect against bacteria and viruses.
M2 macrophages are induced by certain cytokines such as
IL-4,
IL-10, and
IL-13. These macrophages are associated with wound healing and tissue repair.
In a normal tissue, the ratio of M1:M2 macrophages is highly regulated. On inflammation, this ratio can be changed.
Markers of macrophages
Macrophages are endowed with a variety of receptors for lineage-determining growth factors, T helper (Th) cell cytokines, and B cell, host, and microbial products
[3]. Examples of proteins expressed by macrophages include CD14,
CD40, CD11b, CD64,
EMR1, lysozyme M, MAC-1/MAC-3, and
CD68. Cytometry or immunohistochemical staining can be used to identify macrophages.
D14, CD68, and EMR1 are widely used as macrophage‐specific markers. But some scientists have demonstrated that among the three expected macrophage-specific markers, only EMR1 shows a strict specificity. Both CD14 and CD68 are expressed in fibroblasts-like cells (adipoblasts), preadipocytes and adipocytes in addition to macrophages[4].
Macrophages in inflammation
The inflammatory response is a complex, highly regulated sequence of events that can be provoked by a variety of stimuli, such as pathogens, noxious mechanical and chemical agents, and autoimmune responses.
Macrophages take part in the autoregulatory loop in the inflammatory process and produce a wide range of biologically active molecules that are involved in both beneficial and detrimental outcomes in inflammation. Therefore, therapeutic interventions targeted macrophages and their products represent an approach to controlling inflammatory diseases[5].
Macrophages in diseases
Diseases and conditions that involve unregulated macrophage plasticity include obesity, insulin resistance and diabetes, tumors, atherosclerosis[6], granulomas, and inflammatory bowel disease.
Some pathogens are able to live inside the macrophage, evading immune attacks. Diseases with this type of behavior include tuberculosis (caused by Mycobacterium tuberculosis), leishmaniasis (caused by Leishmania species), and Chikungunya (caused by CHIKV or Chikungunya virus).
Reference:
[1] Evanna L. Mills et al, Itaconate is an anti-inflammatory metabolite that activates Nrf2 via alkylation of KEAP1,
Nature (2018).
[2] Dmitry A. Ovchinnikov, Macrophages in the embryo and beyond: Much more than just giant phagocytes,
Genesis (2008).
[3] Fernando O. Martinez et al, The M1 and M2 paradigm of macrophage activation: time for reassessment,
F1000Prime Reports (2014).
[4] Wael Khazen et al, Expression of macrophage-selective markers in human and rodent adipocytes,
FEBS Letters (2005).
[6] Samina Bashir et al, Macrophage polarization: the link between inflammation and related diseases,
Inflammation Research (2016).
CUSABIO team. Itaconate is a negative regulator of inflammation. https://www.cusabio.com/c-20549.html
Comments
Leave a Comment