FAP may be a drug target for pancreatic cancer
Novel drug target for pancreatic cancer
Fibroblast activation protein (FAP) may be a novel drug target for pancreatic cancer, according to a study (Fibroblast activation protein augments progression and metastasis of pancreatic ductal adenocarcinoma) published in the Journal of Clinical Investigation Insight on October 5, 2017[1].
Pancreatic cancer, which forms in the pancreas, is very hard to control. One problem is that pancreatic cancer is rarely detectable in its early stages. Pancreatic cancer generally spreads rapidly, and symptoms don't appear until it's too late. The prognosis of pancreatic cancer patients remains dismal, with a 5-year survival rate of only about 5%.
FAP, which is a transmembrane cell surface proteinase, belongs to the serine protease family. Expression of FAP has been detected in cancer-associated fibroblasts of many human cancers, such as pancreatic cancer, breast cancer, colorectal cancer, and cervical cancer. Some studies uncovered that FAP depletion suppresses cancer cell proliferation and metastasis in experimental animals.
For the current study, a team consisting of researchers from the University of Pennsylvania in the USA, National Yang-Ming University School of Medicine, and Academia Sinica in Taiwan further explored the role of FAP in pancreatic cancer. Using immunofluorescent staining method, the team examined FAP expression in clinical specimens collected from patients with pancreatic cancer and discovered that the level of FAP was much higher in stromal cells in pancreatic tumors than that in adjacent normal pancreatic tissues. Similar results were found in FAP luciferase reporter knockin mice. Investigating the association between FAP level and patient outcome, the team found that high FAP level could predict shorter survival.
Next, the team carried out experiments in mouse models of pancreatic cancer. The results suggested that FAP is not essential for the initiation of pancreatic cancer but is critical for promoting the progression of pancreatic cancer. Deletion of FAP prolonged the animals' survival. Furthermore, the study indicated that FAP expression by stromal and/or tumor cells could contribute to the resistance of pancreatic cancer to necrotic cell death and could drive the spread of cancer cells to multiple visceral organs.
To conclude, the data support a role of FAP in augmenting progression and metastasis of pancreatic cancer. Therefore, FAP might be a new target for drug therapy in this deadly disease.
Dr. Ellen Puré, a professor at the University of Pennsylvania School of Veterinary Medicine and the corresponding author of this study, noted that their study is the first to demonstrate that FAP contributes to metastasis.
The laboratory of Dr. Puré is focusing on the cellular and molecular basis of inflammation and fibrosis. Their recent studies explore the function of FAP and other molecules in human disease.
Cause and risk factors of pancreatic cancer
The exact cause of pancreatic cancer is not known. Doctors are usually unable to tell why a specific patient developed pancreatic cancer. It's well established that cancer is characterized by uncontrolled cell growth driven by DNA damage. Only 5%-10% of all cases of pancreatic cancer report a family history. While the genetic basis for the majority of the familial clustering of pancreatic cancer remains unclear, several pancreatic cancer susceptibility genes have been established or suggested, such as
BRCA2,
STK11/LKB1,
PALB2,
PRSS1,
SPINK1,
CDKN2A,
BRCA1,
CFTR, and the ABO blood group locus
[2].
In addition to genetic factors, there are many other risk factors for the disease. Here is a list of confirmed and suspected risk factors for pancreatic cancer
[3][4].
1. A family history
2. Older age
3. Smoking
4. High alcohol intake
5. Dietary factors
6. Diabetes
7. Chronic pancreatitis
8. Exposure to toxic substances
9. Previous peptic ulcer
10. Organ transplant
11. Overweight or obesity
12. Sedentary lifestyle
13. Hepatitis
14. Breast and ovarian cancer syndrome
15. Other serious diseases
Pancreatic tumors have profoundly oncogenic alterations, which occur in high frequencies. These alterations drive growth and cell survival and alter the metabolism of pancreatic cancer. There are also rare alterations, that are found in effectively unique combinations in each patient. All these genetic alterations may imply an ability to rapidly develop acquired resistance to therapies[5].
Invasive nature of pancreatic cancer
During the past several decades, there has been an overall reduction in cancer-related death in developed countries, in particular for lung, breast, colorectal and prostate cancer. However, for pancreatic cancer, the mortality rates are increased. Pancreatic cancer is a highly aggressive cancer that kills more than half of all its victims within 6 months after diagnosis. Nearly all diagnosed patients ultimately succumb to the disease. Why is pancreatic cancer so lethal? There are several reasons:
1. Rapid progress
2. Lack of early signs
3. Late diagnosis
4. Low resection rate
5. Lack of efficacious therapies
6. Incomplete knowledge of etiology
Pancreatic cancer often grows fast and spreads microscopically early in the disease course. When diagnosed, only 7% of pancreatic cancers are considered localized disease, which is alarmingly low compared to other cancers[6]. This means that most patients with pancreatic cancer are not suitable to undergo a surgery because their cancer has spread from its primary site to distant organs and complete resection of tumors by surgery is usually impossible.
Our understanding of what drives the development and metastasis of pancreatic cancer is far from complete. There is a lack of markers of early detection as well as a lack of targets for treatment. At the early stage of pancreatic cancer, symptoms such as weight loss, abdominal pain, the onset of diabetes, unexplained jaundice, and unprovoked thrombosis may occur. However, these symptoms are non-specific and may also appear in other diseases.
For breast, prostate, melanoma, and testicular cancers, simple examinations can evaluate the condition. In contrast, the pancreas is buried deep in the abdomen behind the stomach, making it hard to access.
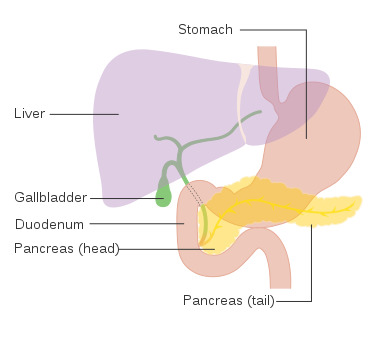
Fig 1. The Pancreas
(By Cancer Research UK - Original email from CRUK, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=34334263)
For these reasons, pancreatic cancer often goes unnoticed until it is too late. Once metastasis occurs, it's hard to treat. For advanced pancreatic cancer, there are still treatment options, but the most efficacious are also the most burdensome.
Recurrence of pancreatic cancer after treatment is another factor that contributes to the dismal prognosis. Despite treatment at early stages, there is a 40% chance of recurrence.
For these reasons, the 5-year survival rate of pancreatic cancer remains quite low. In fact, pancreatic cancer is one of the leading cause of cancer-related death worldwide. According to estimates, pancreatic cancer accounts for about 3% of all cancers in the US and 7% of all cancer deaths.
Fig. 2 Metastasis and prognosis of pancreatic cancer compared with other cancers
|
Type of cancer
|
Percentage of localized disease at diagnosis
|
5-year survival rate
|
|
Pancreatic cancer
|
7%
|
5%
|
|
Breast cancer
|
61%
|
17%
|
|
Colon cancer
|
40%
|
60%
|
|
Lung cancer
|
16%
|
10%
|
|
Ovarian cancer
|
19%
|
45%
|
|
Prostate cancer
|
91%
|
99%
|
Reference:
[2] Alison P. Klein, Genetic susceptibility to pancreatic cancer,
Molecular Carcinogenesis (2011).
[4] Ramesh Khadka et al, Risk factor, early diagnosis and overall survival on the outcome of association between pancreatic cancer and diabetes mellitus: Changes and advances, a review,
International Journal of Surgery (2018).
[6] Chengfei Zhao et al, Pancreatic cancer and associated exosomes,
Cancer Biomarkers (2017).
CUSABIO team. FAP may be a drug target for pancreatic cancer. https://www.cusabio.com/c-20391.html
Comments
Leave a Comment