Infection Immunity
Infection immunity aims to study the interaction between the host and pathogenic microorganisms. After a pathogen infects the body, on the one hand, the body's cells quickly stimulate immune regulation signals through the immune recognition system, and then respond through innate immunity and acquired immunity, thereby resisting the invasion of external microorganisms. On the other hand, pathogenic microorganisms can evolve escape mechanisms to evade immune system surveillance. Here, we take virus as an example to illustrate infection immunity.
1. How does the Human Body's Immunity Fight against Viral Infection?
Virus, the simplest living organisms except viroid, is composed of nucleic acids and protein capsids that wrap the nucleic acids. The virus completely relies on the biosynthetic system of the host cell to replicate the viral protein and its genetic material and assemble the virion. The virus uses cell surface receptors to infect cells, many of which are related to the immune system. After the virus successfully infects the host cell, its genetic material is exposed to the cytoplasm and begins to guide the synthesis of viral macromolecules and the assembly of virions (Figure 1).
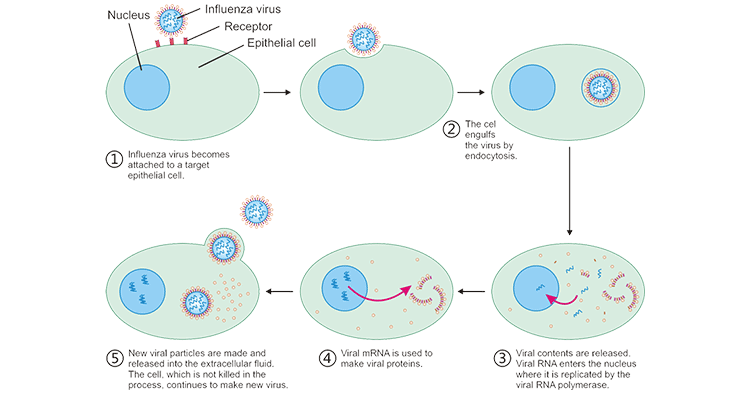
Figure 1. The Cycle of virus infected host cell
A few viruses such as CMV can coexist peacefully with host cells and parasitize for a long time, which are called non-cytotoxic viruses. But, most viruses are cytotoxic viruses, and their intracellular propagation and parasitism quickly lead to the death of host cells and eventually cause a series of infectious diseases. The body's defense against virus infection is mainly divided into three sections. One is to inhibit virus replication and reproduction in host cells by secreting cytokines (such as IFEN and TNF); the other is to kill virus-infected host cells through NK cells and CTL. ; The third is to block the ability of the virus to infect cells by neutralizing antibodies. These three sections can be summarized as innate and adaptive immunity.
2. What is the Innate Immune Response to Viral Infection?
In viral infections the host innate immune system is meant to act as a first line defense to prevent viral invasion or replication before more specific protection by the adaptive immune system is generated. In the innate immune response, pattern recognition receptors (PRRs) are engaged to detect specific viral components such as viral RNA or DNA or viral intermediate products and to induce type I interferons (IFNs) and other pro-inflammatory cytokines in the infected cells and other immune cells. In 2008, Shohei Koyama et al. have summarized these innate immune receptors and their unique downstream pathways according to numerous studies [1]. They summarized these recognition receptors roles in the innate immune response to virus infection from RNA sensing and DNA sensing (Figure 2).
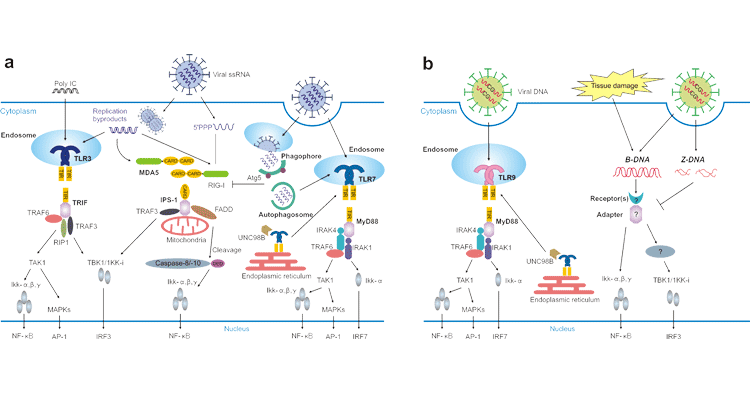
Figure 2. RNA (a) and DNA (b) sensing in virus infection
*this picture is derived from reference 1.
3. What is the Adaptive Immune Response to Viral Infection?
The adaptive immune response is an antigen-specific immune response that takes days to weeks to develop. The initiating event in the induction of the adaptive immune response is the activation of naïve T cells through antigen presentation [2]. Viruses can infect cells by combining the receptor molecules on their surface with corresponding molecules on the surface of host cells. The specific antibodies produced by the body against the surface molecules of invading viruses play an important role in the prevention and treatment of viral infections. These antibodies can act on the virus in the body fluids in the early stage of infection and the virus released after the lysis of the infected cells.
The antiviral effects of antibodies are reflected in the following aspects: 1. Neutralize virus infectivity: the binding of antibodies to virus surface proteins can block its contact with cell surface receptors or interfere with virus invasion into cells, mucosal surface IgA molecules The role in this aspect is particularly important; 2. Sensitized virus particles: After the antibody binds to the virus, the virus particles are directly lysed by activating complement, and the complement fragments such as C3a and C5a produced in the process chemoattract leukocytes; 3. Mediate antibody-dependent Cytotoxicity-ADCC: Some viral membrane proteins can be expressed on the surface of infected host cells. Virus-specific antibodies mark the infected cells by identifying these viral proteins, and induce NK cells and megacells to kill these cells.
4. Featured Targets Related to Infection Immunity
CUSABIO collects and lists related molecules/targets of infection immunity, click to see all the related molecules/targets and research reagents of them.
References
[1] Shohei Koyama; Ken J. Ishii; Cevayir Coban; et al. Innate immune response to viral infection [J]. 2008, 43(3), 0–341.
[2] JANE E. LIBBEY and ROBERT S. FUJINAMI. Adaptive immune response to viral infections in the central nervous system [J]. Handb Clin Neurol. 2014; 123: 225–247.


