Epstein-Barr virus
Epstein-Barr virus (EBV), also known as human herpesvirus 4, is a member of the herpes virus family. It is one of the most common human viruses. EBV is found worldwide and is a common cause of viral pharyngitis, especially in young adults. Most people get infected with EBV at some point in their lives without even knowing it. EBV spreads most commonly through bodily fluids, primarily saliva. EBV can cause infectious mononucleosis, also called mono, and other illnesses.
Read on to learn more about EBV, including structure, the important proteins, infection mechanisms, infection Symptoms, transmission, Diagnosis and Treatment.
The Structure of Epstein-Barr virus
Epstein-Barr virus is about 122–180 nm in diameter and is composed of a double helix of deoxyribonucleic acid (DNA) which contains about 172,000 base pairs and 85 genes. [1] The DNA is surrounded by a protein nucleocapsid, which is surrounded by a tegument made of protein, which in turn is surrounded by an envelope containing both lipids and surface projections of glycoproteins, which are essential to infection of the host cell.[2]
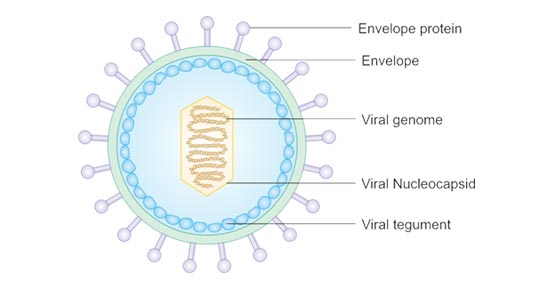
Figure 1. The structure of EBV
Proteins of Epstein-Barr virus
Epstein-Barr virus Infection mechanisms
Epstein-Barr virus (EBV) infection occurs by distinct mechanisms across different cell types. EBV can infect both B cells and epithelial cells.
To enter B cells, viral glycoprotein gp350 binds to cellular receptor. Then, viral glycoprotein gp42 interacts with cellular MHC class II molecules. This triggers fusion of the viral envelope with the cell membrane, allowing EBV to enter the B cell.[4] Human CD35 is an additional attachment factor for gp350/220, and can provide a route for entry of EBV into CD21-negative cells, including immature B-cells. Once EBV's initial lytic infection is brought under control, EBV latency persists in the individual's B cells for the rest of their life.
To enter epithelial cells, viral protein BMRF2 interacts with cellular β1 integrins. Then, viral protein gH/gL interacts with cellular αvβ6/αvβ8 integrins. This triggers fusion of the viral envelope with the epithelial cell membrane, allowing EBV to enter the epithelial cell.[4]
Transmission of Epstein-Barr virus
EBV spreads most commonly through bodily fluids, especially saliva. EBV is spread by saliva through kissing, sharing drinks and food, using the same cups, eating utensils, or toothbrushes, having contact with toys that children have drooled on. The virus probably survives on an object at least as long as the object remains moist.
However, EBV can also spread through blood and semen during sexual contact, blood transfusions, and organ transplantations.
How to confirm EBV infection
EBV infection can be confirmed with a blood test that detect specific antibodies to EBV, including:
- Viral capsid antigen (VCA). Antibodies to VCA appear early in the infection. One type (anti-VCA IgM) disappears after several weeks while another (anti-VCA IgG) persists for life.
- Early antigen (EA). Antibodies to EA appear during an active infection. They typically become undetectable after several months, although they may persist for longer in some people.
- EBV nuclear antigen (EBNA). Antibodies to EBNA slowly appear in the months following infection and can be detected throughout a person's life.
References
[1] Amon W, Farrell PJ (November 2004). "Reactivation of Epstein-Barr virus from latency". Reviews in Medical Virology. 15 (3): 149–56. doi:10.1002/rmv.456. PMID 15546128.
[2] Odumade OA, Hogquist KA, Balfour HH (January 2011). "Progress and problems in understanding and managing primary Epstein-Barr virus infections". Clinical Microbiology Reviews. 24 (1): 193–209.
[3] Entrez Gene: CR2 complement component (3d/Epstein Barr virus) receptor 2". Archived from the original on 2010-12-05.
[4] Tagliavini E, Rossi G, Valli R, Zanelli M, Cadioli A, Mengoli MC, et al. (August 2013). "Lymphomatoid granulomatosis: a practical review for pathologists dealing with this rare pulmonary lymphoproliferative process". Pathologica. 105 (4): 111–6.

