T Cell Cytokines
T cells, referred to as T lymphocytes, are lymph stem cells derived from bone marrow. After differentiation and development in the thymus, they are distributed to immune organs and tissues throughout the body through lymphatic and blood circulation to exert immune functions. The release of cytokines is critically important to many aspects of T cell function. IL-1 is involved in T cell activation. IL-2 is a potent T cell growth factor which is essential for the long-term proliferation of activated T cells. T cell can be divided into several subsets, and they can be distinguished by their unique cytokine production profiles and their functions.
In this article, we will introduce the subsets of T cell and their secreting cytokines in brief. There are 4 main types of T cells, including CD4+ helper cells, CD8+ cytotoxic cells, memory T cells and natural killer T cells.
CD4+ Helper Cells
CD4+ helper cells, also known as Th cells, help in the maturation of B cells into plasma cells and memory B cells. They also assist to activate cytotoxic T cells and macrophages. Naive CD4+T cells are activated after interaction with antigen-MHC complex and differentiate into specific subsets depending on the cytokine milieu of the microenvironment. Besides the classical T-helper 1 (Th1) and T-helper 2 (Th2), other subsets have been identified, including T-helper 17 (Th17) and regulatory T cell (Treg), each with a characteristic cytokine profile.
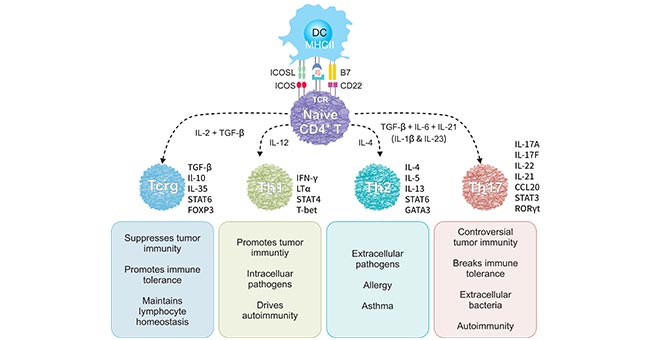
Figure 1. The main subsets of CD4+ helper cells and their function.
Th1 cells predominantly produce interferon-γ (IFNγ) and play an important role in protective immune responses to intracellular viral and bacterial infection. Th2 cells are critical for expelling extracellular parasites by secreting IL-4, IL-5, IL-9, IL-13, and IL-25. Th17 cells are responsible for controlling extracellular bacteria and fungi via producing IL-17A, IL-17F, and IL-22. Treg are important in maintaining immune tolerance, as well as in homeostasis, activation and function.
CD8+ Cytotoxic Cells
CD8+ cytotoxic cells, also known as Tc cells, play a major role in cell mediated immunity, to destroy virally infected cells and tumour cells. They are also involved in transplant rejection. Tc cells recognize their targets by binding to antigen associated with MHC Class I molecules which are present on the surface of all nucleated cells. The affinity between CD8 and the MHC molecule helps in keeping the Tc cell and the target cell bound closely together during antigen-specific activation. When a CD8+ T cell recognises its antigen and becomes activated, they secrete several cytokines, primarily TNF-α and IFN-γ, which have anti-tumour and anti-viral microbial effects.
Memory T Cells
pMemory T cells are long-lived and can quickly expand to large numbers of effector T cells upon re-exposure to the antigen. They provide the immune system with “memory” against previously encountered pathogens. Memory T cells may be either CD4+ or CD8+.
Upon stimulation with their cognate antigen, naive T cells undergo proliferation and differentiation into effector cells, followed by apoptosis or survival as precursors of long-lived memory cells. These phases of a T-cell response and the ensuing maintenance of memory T cells are shaped by cytokines, most notably IL-2, IL-7, and IL-15 that share the common γ chain (γc ) cytokine receptor.
Natural Killer T Cells
Natural Killer T cells, also known as NKT cells, are bridge between the adaptive immune system and the innate immune system. although most T cells function based on recognition of MHC class molecules, NKT cells are able to recognize other antigen classes. NKT cells can be divided into two main subsets based on their TCR diversity and antigen specificities, type I NKT and type II NKT.
Type I NKT cells can release various cytokines such as IL-2, IL-12, and IFN-γ leading to activation and expansion of NK cells into lymphokine-activated killer (LAK) cells. These LAK cells upregulate the effectors or adhesion molecules such as perforin, NKp44, granzymes, FasL, and TRAIL and secrete IFN-γ to adhere and lyse tumor cells. Type II NKT cells can be distinguished from type I NKT cells by their predominance in humans versus mice, TCR binding and distinct antigen specificities.

